
Monkeypox is a hot topic in the medical community recently. This is a virus that is similar to that of smallpox, but has a much lower mortality rate.
The transmission of monkeypox can occur from animal to human or from human to human. If a person is in direct contact with the bodily fluids of an infected animal or is bit by the animal, then they can become infected. Human-to-human transmission occurs through direct contact with infected sores, bodily fluids, respiratory secretions through prolonged face to face contact, or fomite transmission from infected linens or clothes. Also of note, the virus can cross the placenta of a pregnant woman to the fetus and affect the baby. A person is considered contagious until all sores have scabbed over and healthy skin is developing over them. This typically takes two to four weeks to occur. After an exposure, symptoms can take anywhere from 4-21 days to appear.
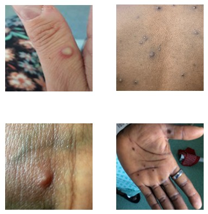
Patients often experience systemic symptoms including fever, headache, sore throat, back pain, myalgia, and fatigue and these symptoms typically last for 1-5 days. The rash usually appears 1-2 days before or 4-5 days after the systemic symptoms. The rash associated with monkeypox progress through several stages. The rash begins as
2-5 mm macules. These eventually develop into papules, vesicles or pseudo-pustules. Lesions usually have a central umbilication. The lesions will eventually crust over and fall off after about 7-14 days from onset. The rash associated with monkeypox is often described as painful, but in the healing phase it can become itchy. There are normally about 1-20 lesions on the body and it is very rare to have over 100 lesions present. The lesions usually appear in the anogenital and perioral areas with small number of lesions on the trunk or acral areas of body. It is uncommon for rash to develop inside the mouth.
For most individuals, monkeypox is a self-limited disease with the symptoms lasting from two to four weeks. However, some patients may develop complications or severe disease. During the 2022 global outbreak, few hospitalizations have been reported and most were for the purpose of isolating the patient. Other reasons for hospitalization included provision of adequate pain management and the need to treat secondary infections.
Suspect monkeypox in a patient who has rash with systemic symptoms, especially if monkeypox is circulating in the community or the patient has traveled to West Africa. If suspected, PCR testing for the orthopoxvirus DNA can be done.
The patient should have two swabs performed on skin lesions and sent to lab for confirmatory testing.
Monkeypox is a self-limited illness for most people and will resolve on its own. Supportive care is recommended and some patient may need pain relief for proctitis or tonsillitis such as stool softeners, topical lidocaine, or sitz baths. Tecovirimat is an antiviral that can be used for treatment in certain cases of monkeypox. Patients warranting treatment include: Those with severe disease such as hemorrhagic disease, confluent lesions, encephalitis, or other conditions requiring hospitalization. Those at risk for severe disease such as those younger than eight years of age, people with a history or presence of atopic dermatitis, persons with other active exfoliative skin conditions, persons who are pregnant or breastfeeding, persons with complications such as secondary bacterial infection, dehydration, or bronchopneumonia; immunocompromised patients. Patients with monkeypox infection in traditionally atypical sites that are usually associated with severe pain. Patients with infection of the eye or eyelids.
If someone has been exposed to monkeypox, they can get post-exposure prophylaxis treatment with one of the orthopoxvirus (smallpox) vaccines within 4 days of the exposure. If a patient warrants vaccine for prevention, they should contact the CDC Emergency Operations Center
(770-488-7100).
